Connect With Us
Blog
Items filtered by date: December 2024
Avoiding Falls in Pickleball

Falls are a common risk in pickleball, affecting both beginners and seasoned players. For newer players, unfamiliarity with movement patterns increases the likelihood of missteps. Experienced players, despite their skills, often face risks due to overconfidence or fatigue during intense games. Wearing proper pickleball-specific shoes is essential for maintaining traction and stability on the court. One key safety tip is to avoid backpedaling when retrieving lobs, as this movement can easily lead to loss of balance. Instead, turning and moving forward is a safer approach. Improving balance and agility through targeted exercises can also significantly reduce fall risks, keeping you steady during sudden directional changes. If a fall has resulted in foot or ankle pain, it is suggested that you consult a podiatrist for timely care and recovery.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Rouder from S.I. Podiatry. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Midfoot Pain Syndrome or Morton’s Neuroma
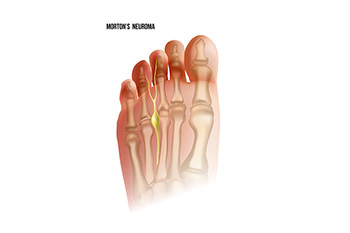
Morton's neuroma, also known as midfoot pain syndrome, is a condition that causes pain in the ball of the foot, usually between the third and fourth toes. It occurs when the tissue surrounding a nerve thickens, leading to irritation or compression. The exact cause of Morton's neuroma is not always clear, but it can result from factors such as wearing tight or poorly fitting shoes, especially those with a narrow toe box or high heels, which put pressure on the toes. Activities that involve repetitive stress or impact, such as running or jumping, can also contribute to the development of the condition. Symptoms include a sharp, burning pain, tingling, or a sensation of something being stuck inside the shoe. The discomfort often worsens with prolonged walking or standing. If you have pain in this part of your foot, it is suggested that you consult a podiatrist who can guide you toward the treatment that is right for you.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Rouder of S.I. Podiatry. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dealing With Peripheral Artery Disease

Peripheral arterial disease, or PAD, is a common complication of diabetes, where poor circulation affects the blood flow to the feet and legs. This reduced circulation can cause the skin to become dry, pale, or even develop ulcers. If left untreated, PAD can lead to serious complications, including infections or amputation. PAD typically results from long-term high blood sugar, which damages blood vessels. The symptoms may include cold feet, slow-healing sores, or numbness. Without proper treatment, the lack of blood flow makes it harder for the body to fight infections and increases the risk of foot ulcers. Once the ulcers form, they can be difficult to heal and are linked to more adverse outcomes, including infections. Regular foot exams, proper wound care, and managing blood sugar levels are key to preventing complications. A podiatrist can help monitor and treat PAD, ensuring the best possible outcomes. If you have foot issues as the result of diabetes, it is suggested that you make an appointment with a podiatrist.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Rouder from S.I. Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Identifying and Treating Seed Corns
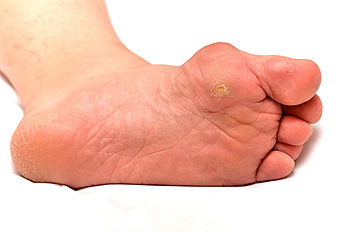
Seed corns, medically known as heloma miliare, are small, well-defined areas of thickened skin that typically form on the soles of the feet. These hard, circular spots are often caused by friction, pressure, or dry skin, and they may appear in clusters. Seed corns are distinct from calluses and plantar warts. Calluses are larger and irregularly shaped, while plantar warts disrupt the skin's natural lines and may include tiny dark dots. Though seed corns are typically painless, they can cause some discomfort, especially in weight-bearing areas of the foot. A podiatrist can diagnose seed corns through a foot examination and distinguish them from other conditions. Treatment includes safely trimming the thickened skin to reduce discomfort, as well as addressing underlying factors like wearing ill-fitting shoes or excessive pressure. Podiatrists also provide guidance on preventive measures, such as selecting proper footwear and using orthotic devices to minimize friction. If you have a problematic corn on your foot, it is suggested that you visit a podiatrist for guidance.
If you have any concerns regarding your feet and ankles, contact Dr. Rouder of S.I. Podiatry. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Managing Leg and Ankle Edema
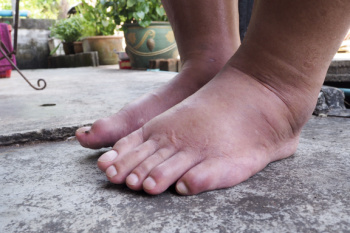
Leg and ankle edema, or swelling, occurs when excess fluid accumulates in the tissues of the lower limbs. This condition is often caused by poor circulation, injury, prolonged sitting or standing, or underlying medical issues like heart, kidney, or liver disease. Edema can be uncomfortable, restrict movement, and, if untreated, can lead to skin infections or sores. Seeing a podiatrist for leg and ankle edema can be beneficial. A podiatrist will assess the underlying causes, which may involve checking circulation, reviewing your medical history, and performing diagnostic tests. This type of doctor can recommend treatments such as compression therapy, elevation techniques, and exercises to reduce fluid buildup. For chronic cases, they might collaborate with other healthcare providers. If you have persistent edema in your lower limbs, it is suggested that you schedule an appointment with a podiatrist who can help you identify underlying causes and provide relief strategies.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact Dr. Rouder of S.I. Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
- Phlebitis - A condition that causes the veins to become inflamed and can also cause leg pain.
- Liver disease - This may lead to low blood levels of albumin which is a protein. This can cause fluid in the blood to pass into the tissues and several areas of the body can become swollen.
- Heart failure - When the heart doesn’t pump properly the blood that is normally pumped back to the heart can pool in the veins of the legs causing swollen feet.
- Kidney disease - One of the main functions of the kidneys is releasing excess fluid in the body. This type of condition can make it difficult for the kidneys to function properly, and as a result the feet may become swollen.
- Deep-vein thrombosis (DVT)- This is a serious condition where blood clots form in the veins of the legs. They can block the return of blood from the legs to the heart which may cause the feet to swell. It is important to be treated by a podiatrist if this condition is present.
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please feel free to contact our office located in Staten Island, NY . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.